Credit: Michael Miller
25 June 2024 Amund Trellevik
Amund Trellevik Ingeborg Eliassen
Ingeborg Eliassen
Antibiotic defences: Ukraine war reignites concerns over global bacteria resistance

Credit: Michael Miller
Antibiotic defences: Ukraine war reignites concerns over global bacteria resistance
25 June 2024Multi-resistant bacteria kill tens of thousands in Europe as the antibiotics don't work. New types are less profitable to develop, so it is not done. Faced with the third biggest threat to public health in Europe, the EU is proposing billions in subsidies to tempt the pharma industry into action.
On instinct, he woke up to the sound of the missile. Almost as if in slow motion, he saw it come through the ceiling and explode in front of him. Then everything went black.
For two days straight, Roman Golub and his Ukrainian military unit had been engaged in fierce fighting with Russian forces near Popasna in Luhansk on that late June evening in 2022. To get a few minutes' rest, Roman walked down into the basement of an abandoned house the soldiers used as a shelter. He rolled out his sleeping mat and closed his eyes.
The soldiers who found him after the attack, estimated a 10 per cent chance of survival. The injuries were extensive. Tourniquets were applied to stop the bleeding. He was evacuated to the nearest collection point a few miles behind the frontline, and within hours he was transported to a hospital near Dnipro. There, life-saving operations began. To ensure Roman wouldn't die from infections, the doctors gave him antibiotics. In large quantities.
“There was no pain, just anxiety and nothing more, the pain came first in the hospital. I wasn't thinking about death when this happened. I only thought about why I could no longer move,” Roman says.
For two days straight, Roman Golub and his Ukrainian military unit had been engaged in fierce fighting with Russian forces near Popasna in Luhansk on that late June evening in 2022. To get a few minutes' rest, Roman walked down into the basement of an abandoned house the soldiers used as a shelter. He rolled out his sleeping mat and closed his eyes.
The soldiers who found him after the attack, estimated a 10 per cent chance of survival. The injuries were extensive. Tourniquets were applied to stop the bleeding. He was evacuated to the nearest collection point a few miles behind the frontline, and within hours he was transported to a hospital near Dnipro. There, life-saving operations began. To ensure Roman wouldn't die from infections, the doctors gave him antibiotics. In large quantities.
“There was no pain, just anxiety and nothing more, the pain came first in the hospital. I wasn't thinking about death when this happened. I only thought about why I could no longer move,” Roman says.

Roman Golub enlisted in the Ukrainian army back in 2014. In the summer of 2022, he was seriously injured in fighting in eastern Ukraine.Private photo
War harms people in the most horrific ways, while at the same time sanitation conditions are miserable and health services are often collapsing. In such situations, wounds quickly become infected. World War 2 accelerated the development of antibiotics, first discovered in 1928, and drastically changed the world for the better: People lived longer and enjoyed better health. Food production in agriculture increased because it became possible to control infections in livestock.
But the increased use of antibiotics over the following decades has led to another major problem: resistance. Bacteria mutate and find ways to protect themselves against antibiotics. That is why research into new types of antibiotics has been crucial to keep up with increasingly complex and dangerous infections.
However, researchers say that no new classes of antibiotics have been brought to market in the last 30 years. Already, 35,000 people in Europe die every year from infections that antibiotics cannot treat. If nothing is done to dramatically increase the development of new antibiotics, 10 million people could die globally each year from multidrug-resistant bacteria by 2050, warns the World Health Organisation.
But the increased use of antibiotics over the following decades has led to another major problem: resistance. Bacteria mutate and find ways to protect themselves against antibiotics. That is why research into new types of antibiotics has been crucial to keep up with increasingly complex and dangerous infections.
However, researchers say that no new classes of antibiotics have been brought to market in the last 30 years. Already, 35,000 people in Europe die every year from infections that antibiotics cannot treat. If nothing is done to dramatically increase the development of new antibiotics, 10 million people could die globally each year from multidrug-resistant bacteria by 2050, warns the World Health Organisation.
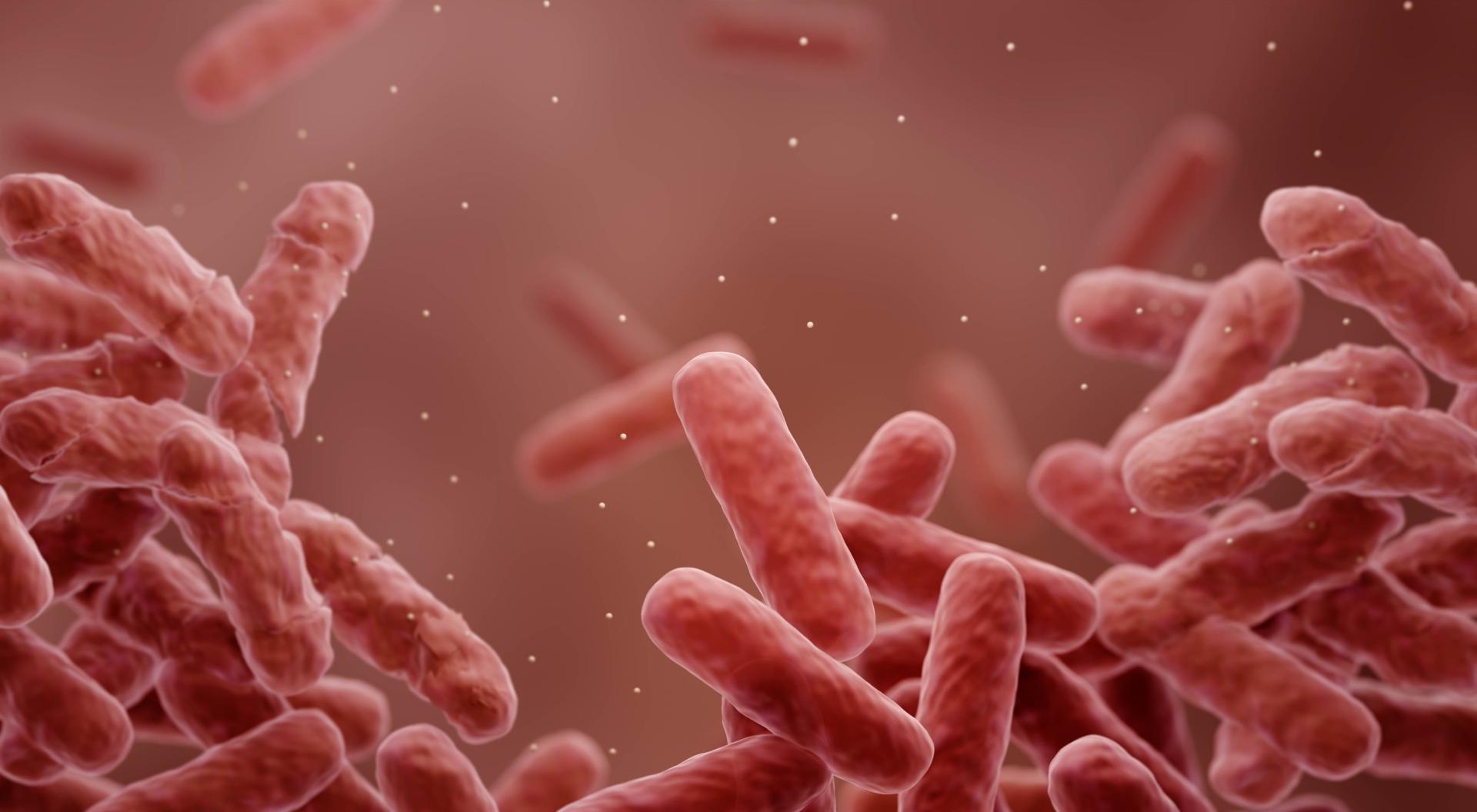
35,000 people in Europe die every year from infections that antibiotics cannot treat.Shutterstock
But the road to new antibiotics is long, complicated - and expensive. The industry itself estimates that each new antibiotic for the European market will cost between €1 billion and €1.5 billion. New antibiotics should be used rarely and only in short courses of treatment. This makes antibiotics of little economic interest to pharmaceutical companies. They earn far more from selling drugs against rare diseases and on novel cancer treatments.
The battle over who will pay to avert a massive public health crisis is underway.
There are growing fears around antimicrobial-resistance (AMR), and conflicts, as seen in Iraq and Afghanistan at the turn of the century, can often bring these risks to the fore. The war in Ukraine has led to multi-resistant bacteria now being discovered in hospitals in northern and western Europe, areas that previously had far fewer cases than elsewhere in Europe due to campaigns to restrict the use of antibiotics.
Roman was part of the first group of soldiers evacuated from Ukraine through the EU Medevac system. When he arrived at Oslo University Hospital in Norway in October 2022, doctors and nurses were covered in infection control outfits, wary of the risky bacteria he might be carrying. They looked like astronauts, he would later recall.
The battle over who will pay to avert a massive public health crisis is underway.
There are growing fears around antimicrobial-resistance (AMR), and conflicts, as seen in Iraq and Afghanistan at the turn of the century, can often bring these risks to the fore. The war in Ukraine has led to multi-resistant bacteria now being discovered in hospitals in northern and western Europe, areas that previously had far fewer cases than elsewhere in Europe due to campaigns to restrict the use of antibiotics.
Roman was part of the first group of soldiers evacuated from Ukraine through the EU Medevac system. When he arrived at Oslo University Hospital in Norway in October 2022, doctors and nurses were covered in infection control outfits, wary of the risky bacteria he might be carrying. They looked like astronauts, he would later recall.

Oleksandra Strelska, a Ukrainian nurse at Oslo University Hospital.

The hospital has treated soldiers from Ukraine whose injures contain multi-resistant bacteria.

Drawings and postcards on the ward where several Ukraine fighters have been treated in Oslo.

Roman was part of the first group of soldiers evacuated from Ukraine through the EU Medevac system. All credits: Michael Miller
“For some [patients], it's a tough experience to realise that we have to protect ourselves from them, that we lose the close human contact,” says Oleksandra Strelska, a Ukrainian nurse at the hospital who also acts as interpreter for those arriving from her home country. "Many people express that they are ashamed of the bacteria they have brought with them from Ukraine. They are so grateful for the help they receive. Some of them buy us chocolate... but we can't accept it because of infection control considerations."
Since the start of the Russian invasion in February 2022, the WHO has documented more than 1,800 attacks on health institutions, including ambulances. European countries joined forces on receiving patients to help the war-torn healthcare system.
A study of bacterial samples from Ukrainian hospitals, carried out by Swedish researchers at Lund University in 2022, showed that six percent of 156 samples were resistant to all antimicrobials tested. In the Netherlands and Germany, researchers made similar findings in Ukrainian patients at the country's hospitals. From 2014 to 2020, war wounds in Ukraine had a higher incidence of multidrug-resistant bacteria compared to Ukrainian civilian hospitals and other European countries, study shows
Since the start of the Russian invasion in February 2022, the WHO has documented more than 1,800 attacks on health institutions, including ambulances. European countries joined forces on receiving patients to help the war-torn healthcare system.
A study of bacterial samples from Ukrainian hospitals, carried out by Swedish researchers at Lund University in 2022, showed that six percent of 156 samples were resistant to all antimicrobials tested. In the Netherlands and Germany, researchers made similar findings in Ukrainian patients at the country's hospitals. From 2014 to 2020, war wounds in Ukraine had a higher incidence of multidrug-resistant bacteria compared to Ukrainian civilian hospitals and other European countries, study shows
“Despite global and regional efforts, considerable gaps remain in our understanding of the magnitude, distribution and trend of drug-resistant infections”
— World Health Organisation
In its latest report from November 2023, the European Centre for Disease Prevention and Control said that the impact of the Ukraine war on AMR is still unknown. But there is "detection of multidrug-resistant organisms in patients recently hospitalised in Ukraine" in many EU/EEA countries.
For the last decade, experts have warned that the overuse of antibiotics and the lack of research and production of new antibiotic classes will inevitably threaten public health. In a few years', infections that we consider harmless today could become fatal.
"Despite global and regional efforts, considerable gaps remain in our understanding of the magnitude, distribution and trend of drug-resistant infections at the national and global level," the WHO writes in its 2022 report on antimicrobial resistance.
For the last decade, experts have warned that the overuse of antibiotics and the lack of research and production of new antibiotic classes will inevitably threaten public health. In a few years', infections that we consider harmless today could become fatal.
"Despite global and regional efforts, considerable gaps remain in our understanding of the magnitude, distribution and trend of drug-resistant infections at the national and global level," the WHO writes in its 2022 report on antimicrobial resistance.
.png&w=3840&q=75)
Investigate Europe
Developing an antibiotic can cost hundreds of millions of euros before they even reach pharmacy shelves. And when they do reach the shelves, it is best they remain there. If antibiotics are overused, it increases the likelihood that they become ineffective over time. Consequently, antibiotic production is financially unattractive for pharmaceutical companies.
"A completely new and fantastic antibiotic… could generate a company revenue of €1.5 billion over its entire life cycle of more than 10 years. This sounds like a lot, but it really isn’t,” says Enrico Baraldi, a business professor at Sweden’s Uppsala University.
“By the time you've spent many years and reached clinical trials, you already have spent up to €50 million. Then you have to spend another €300 million on clinical trials and post-approval costs, knowing there is a 60 to 70 per cent chance of failure.”
The big companies have largely left the antibiotics industry, says Christine Årdal, researcher at the Norwegian Institute of Public Health. “There are only three large companies that have antibiotics in clinical development.”
"A completely new and fantastic antibiotic… could generate a company revenue of €1.5 billion over its entire life cycle of more than 10 years. This sounds like a lot, but it really isn’t,” says Enrico Baraldi, a business professor at Sweden’s Uppsala University.
“By the time you've spent many years and reached clinical trials, you already have spent up to €50 million. Then you have to spend another €300 million on clinical trials and post-approval costs, knowing there is a 60 to 70 per cent chance of failure.”
The big companies have largely left the antibiotics industry, says Christine Årdal, researcher at the Norwegian Institute of Public Health. “There are only three large companies that have antibiotics in clinical development.”
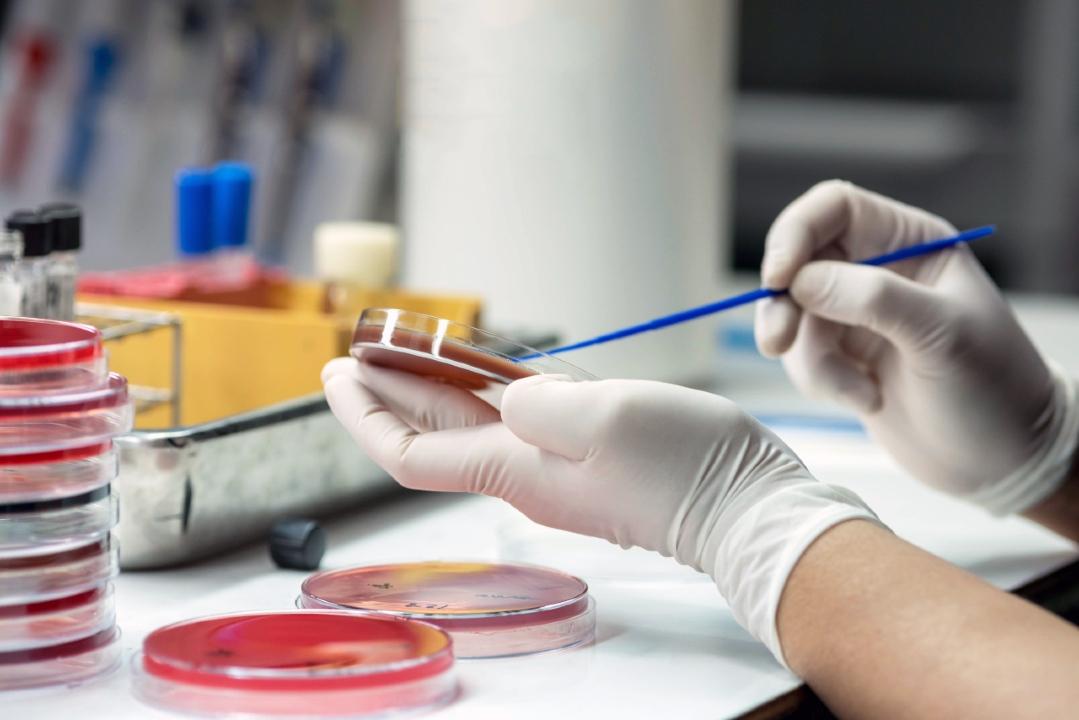
Antibiotic development can cost hundreds of millions of euros before the new drugs even reach pharmacy shelves. Shutterstock
In 2016, over 100 companies and organisations signed the Davos Declaration at the World Economic Forum to “reduce the development of antimicrobial resistance”, invest in new research and improve access to antibiotics. Novartis, the Swiss pharmaceutical giant, signed the document. In 2018, however, the company shut down its AMR research centre in the US.
At the time Novartis said the “commercial model for anti-infectives is critically challenged” and questioned whether “large pharma can sustainably support” investments in the area. Novartis told Investigate Europe that the firm supports several initiatives aimed at reducing AMR globally.
The pharmaceutical industry is backing a proposal from the European Commission to tempt companies with billions in revenue to develop new antibiotics. The proposal is now facing opposition.
Experts warn in particular against a proposed voucher system that would give companies an extended monopoly on blockbuster drugs, in exchange for developing new antibiotics.
At the time Novartis said the “commercial model for anti-infectives is critically challenged” and questioned whether “large pharma can sustainably support” investments in the area. Novartis told Investigate Europe that the firm supports several initiatives aimed at reducing AMR globally.
The pharmaceutical industry is backing a proposal from the European Commission to tempt companies with billions in revenue to develop new antibiotics. The proposal is now facing opposition.
Experts warn in particular against a proposed voucher system that would give companies an extended monopoly on blockbuster drugs, in exchange for developing new antibiotics.
“You cannot expect commercial companies to develop medicines that they subsequently are not expected to market in high volumes. You need a different way of financing new antibiotic drug development.”
— Ellen 't Hoen
Such a system would be very costly for European countries. It would force countries to pay for antibiotics that they are not guaranteed access to. And it would delay access to generics or biosimilar drugs, says Årdal, who adds that it is urgent to put in place new financing methods. One solution, argues Årdal, could be subscription models for countries to antibiotics. In this way, companies are guaranteed income over time. And states are guaranteed access when they need it.
The proposal is now on its way through the EU system. The elected representatives in the EU Parliament want to reduce big pharma's ability to extend monopolies on innovative medicines.
“This is spending that will come on top of already overburdened health budgets," says Tilly Metz, a Luxembourg Green MEP.
Some call this situation a market failure. But that's exactly how the market works, says Ellen 't Hoen, an expert on the pharmaceutical industry. “You cannot expect commercial companies to develop medicines that they subsequently are not expected to market in high volumes. You therefore need a different way of financing new antibiotic drug development.”
The proposal is now on its way through the EU system. The elected representatives in the EU Parliament want to reduce big pharma's ability to extend monopolies on innovative medicines.
“This is spending that will come on top of already overburdened health budgets," says Tilly Metz, a Luxembourg Green MEP.
Some call this situation a market failure. But that's exactly how the market works, says Ellen 't Hoen, an expert on the pharmaceutical industry. “You cannot expect commercial companies to develop medicines that they subsequently are not expected to market in high volumes. You therefore need a different way of financing new antibiotic drug development.”
Frederic Peyrane is the managing director of Beam Alliance, an association of small and medium-sized enterprises in Europe in the field of AMR. Regardless of the mechanism, enough money must be put on the table. The voucher proposal alone from the European Commission will not be sufficient, says Peyrane.
The industry itself has a responsibility to attract investors, Peyrane admits. "We should not overestimate investors' willingness to understand the mechanisms behind the development of antibiotics. We need something that can be explained to people who don't really want to spend a lot of time on this, and who compare antibiotics to investing in new cancer drugs," says Peyrane.
The proposed voucher system is "unfair for consumers, because it would delay access to cheaper generics to treat other diseases and would come at a huge cost to public health systems", says Ancel·la Santos from the European Consumer Organisation.
The industry itself has a responsibility to attract investors, Peyrane admits. "We should not overestimate investors' willingness to understand the mechanisms behind the development of antibiotics. We need something that can be explained to people who don't really want to spend a lot of time on this, and who compare antibiotics to investing in new cancer drugs," says Peyrane.
The proposed voucher system is "unfair for consumers, because it would delay access to cheaper generics to treat other diseases and would come at a huge cost to public health systems", says Ancel·la Santos from the European Consumer Organisation.

Roman and his wife Lena in Oslo. Credit: Michael Miller

He attends an anti-war demonstration in the Norwegian capital. Credit: Michael Miller
This need for innovation was witnessed first-hand by the Norwegian doctors who were treating Roman, the Ukrainian soldier. His body contained bacteria that hospital staff had rarely seen. The solution was to retrieve antibiotics from the 1960s and 1970s, drugs with such severe side effects that doctors today are refraining from use.
"We had to order antibiotics that had never previously been used in Norway. Not only are they very expensive. They're also difficult to get hold of,” says Kristian Tonby, a senior consultant at the Department of Infectious Diseases at Oslo University Hospital.
Roman has now been discharged from the hospital. He is walking on his own two feet, which his wife Lena says is a miracle considering the injuries he sustained. His days in the Norwegian capital are spent rehabilitating - and participating in anti-war demonstrations.
As soon as doctors allow him, Roman will head back to Ukraine, eager to use his experience to train other soldiers. They won't give up the fight against Russia. But in the fight against resistant bacteria, they are powerless.
Editor: Chris Matthews
"We had to order antibiotics that had never previously been used in Norway. Not only are they very expensive. They're also difficult to get hold of,” says Kristian Tonby, a senior consultant at the Department of Infectious Diseases at Oslo University Hospital.
Roman has now been discharged from the hospital. He is walking on his own two feet, which his wife Lena says is a miracle considering the injuries he sustained. His days in the Norwegian capital are spent rehabilitating - and participating in anti-war demonstrations.
As soon as doctors allow him, Roman will head back to Ukraine, eager to use his experience to train other soldiers. They won't give up the fight against Russia. But in the fight against resistant bacteria, they are powerless.
Editor: Chris Matthews